Conversations at the hospital

When Florence, my mother aged 105 years was first admitted into hospital in July 2019 she had been diagnosed as having two small fractures in the lower half of her left leg and was fitted with a sizeable leg plaster. She spent 10 days or so on the fracture ward and was then discharged on a temporary basis to a ward within a local care home. She was in the care home for about 11 days before she had an ‘episode’. She had become very distressed when being put back to bed from a wheelchair via a hoist. The carers and nurses had called for medical emergency help as she had seemed very distressed and her vital signs – pulse, blood pressure etc had gone into free fall.
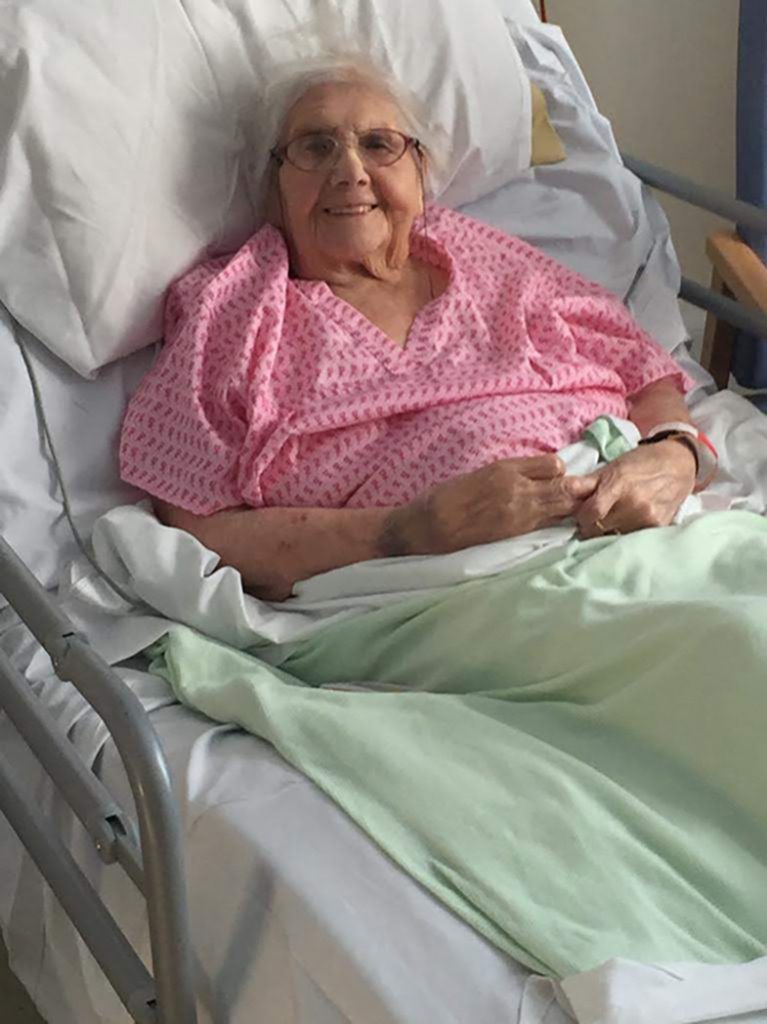
Florence was admitted back into the Accident and Emergency unit of the hospital that she had been discharged from just a short time previously. She spent the night in a cubicle in the A&E unit having been put on an intravenous saline drip and given continuous oxygen. I was very upset to find her in this state when I arrived the following morning. However, the cubicle and the bed she was in were not too uncomfortable and she seemed in a semi-alright state. She was very sleepy, but seemed to have some understanding of what was happening to her and after a few hours she was admitted to one of the wards. This time it was to a ward for elderly people and I was pleased to note that the rather depressing title ‘geriatric ward’ was no longer used. She remained in the ward for a good number of weeks.
The centre for elderly medicine was in a different part of the hospital to the A&E and my sister, my sister-in-law and I walked alongside my mother as she was wheeled in her bed from one part of the hospital to the other. As we turned into the corridor leading to the elderly centre there was a long, painted mural on the wall leading to the stairs and the lift that would take us to the ward Florence was being admitted to. The mural depicted a peaceful and rather lovely English rural scene. It took up the whole of one side of the corridor. It began with a rural setting of fields and trees beside a winding river. As we walked along the corridor alongside the mural, we reached the other side of the fields. Here there was an old country church and beyond the church was the church yard filled with old grave stones and Yew trees. As an entrance to the ward, it felt a bit like Dante’s Divine Comedy and ‘Abandon hope all ye who enter here’.

We entered the ward via a short corridor of kitchens on one side and sluice rooms on the other. This lead into a much wider corridor stretching out to the left, where the four bed women’s side wards or bays were based and to the right a similar arrangement for the men’s ward. In the middle between the two was a station for the nurses and administrators and behind this the ward office. The ward was quite new and seemed well planned. Each small bed unit was bright and airy, clean and reasonably spacious.
Florence settled quite well into the ward and its routine. She seemed comfortable most of the time and not in any pain. She still had her leg in plaster and this would stay in situ for quite a number of weeks to come, with just one visit to the fracture clinic for a change to a slightly less heavy plaster. She slept for much of the time. She was turned from side to side and made more comfortable every few hours. We took in a large pile of nighties and she was kept clean and fresh looking. The nurses and doctors were kind, thoughtful and helpful to her and to us throughout her stay on the ward. They all seemed to like the fact that they had a 105 year old on the ward and one who would often wake up and smile at them when they called her name and almost always answer “I’m alright thank you “ when asked how she was.
Florence could now only eat or drink with a lot of help and a lot of encouragement to stay awake. She still enjoyed much of her food, particularly rice pudding, ice cream and the occasional piece of cake, which she had become increasingly fond of as she got older and that had not faded altogether at this time.
We tried to get someone, family or friend, to visit each day. My sister and I travelled quite a distance, so my sister stayed each weekend at her flat and I usually came on one or two week days early on the train and stayed for the day. It was quite an experience being on the ward for whole days and getting into the rhythm of the hospital day – wash times. meal times, doctors’ rounds, medicine rounds, social worker rounds. These latter visits by the ward social workers took place regularly and mainly seemed to be about sorting or not managing to sort, care arrangements for patients who were ready to go home or to transfer to other care settings. When I visited, Florence slept for most of the time I was there. Periodically I would try and engage her in conversation and always help her to eat at mealtimes. But a large part of our time together was spent with her asleep and me sitting next to her. Sometimes it was difficult to tell if she knew I was there or not.
I found reading to pass the time was a bit difficult. So, I decided that while trying to be very respectful and appreciate everyone’s privacy, I would start making some notes about stuff going on around me and conversations I constantly overheard and was sometimes a part of. The few names that are used have been changed. The following is mainly what I saw and heard while sitting next to Florence.
From the men’s end on almost every visit for the first two weeks, an elderly man could be heard constantly calling “Help, help, will somebody help me” at the top of his voice. He went on and on and on, not faltering or stopping and hardly changing the tone of his voice. Occasionally it would get louder, occasionally quieter, but still it went on. On the second all day visit I wandered down to the men’s half of the ward to see if I could get some sense of what the problem was, if there was a problem. Everything was calm down that end of the ward. I couldn’t quite see where the man was but nobody seemed to be disturbed by his calling or to feel there was any need to try and comfort him or stop him. I thought I heard someone talking to him in one short lull but he very soon started again. By the end of four days listening to this I decided that was what he did and staff had decided that everyone just had to get used to it.
The doctors and nurses, health assistants, dinner servers and care staff were in the main calm and helpful. A few of them seemed to find things like feeding patients rather frustrating and indeed it was, particularly with someone like Florence who fell asleep between almost every mouthful. Occasionally when I visited one or more of the other patients in my mother’s bay would tell me that the young nurses gave up feeding her too quickly and didn’t have enough patience. I thanked them for telling me, but I felt she was probably getting as much as she wanted. The food itself was good and well cooked and she rarely objected to any of the tastes or textures she was offered. Her mouth opened like a little bird when she managed to rouse herself and respond to the offers of food being made. But it was very touching the way those of Florence’s bed fellows who were able to observe what was going on, looked out for her. She herself was not able to communicate with them and they seemed nervous of approaching her, though I wondered if they perhaps did attempt some more communication when I or one of the family were not there.
There was a woman in one of the other bays who wandered up and down the ward continuously. She was looking for her husband and asking us all if we had seen him. She was a relatively young, fit looking woman, white haired, slim and usually wearing jeans and a sweater. She would come into each bay looking for him, sometimes even seeming to look behind chairs or bedside tables. The nurses were very kind to her. They would talk to her and walk around doing their work often with her in tow. Sometimes one or other of the more mobile patients would walk up and down with her and talk with her. A few times while I was there a man, who I presumed was her husband, did come in to visit and take her out. She looked very happy then. She held his arm as he walked her out of the ward and then back in again after an hour or so and her usual look of anxiety had left her for a while. But it quickly restarted after he left and her search began again.
On our first day there, the woman sitting up in her arm chair by the window bed on the other side to Florence tells me and everyone else, that she’s going home that day. She’s talkative and friendly says she was born and bred locally and I realise quickly that going home is her major topic of conversation. She is quite a tall person and beyond being helped in and out of bed to sit in the armchair next to her bed she has limited mobility. She seems very elderly and to have only one tooth. Each afternoon her elderly son visits. He is a big man with quite a noticeable limp and he has some difficulty walking. He uses two sticks and makes his way slowly to her chair and sits next to her. He begins the afternoons conversation on our first day and on each subsequent visit, by responding to her immediate, request to go home. She’s not going home he tells her, as the social worker has not yet managed to find the right sort of care. When she hears this her whole friendly manner changes.
She’s cross. She says “they’re just taking our money and I’m sitting here doing nothing when I could be at home having a nice glass of whisky.” “I just eat their food, I hate them. I want to go home.”
Her son responds in much the same way each day “You can’t go home you need carers to wash you in the morning and put you to bed and they haven’t been able to organise that yet.” “Any fool can put themselves to bed” says his mother. “They’re driving me crazy. They’ve got a bloody cheek keeping me here and its driving me mad.” “It’s driving me mad too” says her son “and you’re driving me mad as well” he says as an aside, before returning to being very patient.
“It’s immoral” she says “and they’ve got a bloody cheek charging me £2 a day for the tele. Blooming too much for me after all the illnesses I’ve had.” “Well you can’t come home yet” her son repeats “we’ve got no care.” “I want to sleep in my own bed. We’re just fitting into their convenience” his mother says.
“I’m very depressed” says her son “We might as well be in timbloodybuctu – and that man’s been shouting every afternoon for 6 weeks- makes you wonder doesn’t it – what’s really happening to him”.
“Don’t waste your energy” says his mother “It’s all useless they won’t do anything”. “Can we go out to the pub?” she says “Or why don’t you just bring me in a bit of whisky?”.
My heart goes out to her at that as I feel a ‘wee dram’ as one of my mother’s carers used to call it might make her feel a lot better. But her son says he’s not allowed to bring it in. I seriously think about offering some from the small bottle my brother has put at the back of Florence’s locker. But then decide it’s probably not very wise. When her son leaves after visiting time his mother returns to telling everyone that she is going home tomorrow and cheers up. A very similar scenario is played out between the two of them on most days that I’m there.
A week or ten days after Florence arrives on the ward, this lady’s care is eventually sorted. She is so happy when she does eventually gather her things to leave with the help of nurses and her son. As she sits in a wheelchair waiting for the hospital transport with her son next to her, I hear her goodbyes to the lady in the next bed. “I shall miss you” she says. If I lived nearer the hospital I’d visit you. But I wish you very well anyway. Its been lovely being next to you and I hope you get home safely very soon… the staff here are lovely”.
The particular lady receiving the goodbyes is immediately opposite Florence’s bed. Most of the time when I am there she seems to be unhappy, uncomfortable and very anxious. Her daughter who visits for about an hour in the afternoon is also very anxious and upset. She talks a lot about the fact that her mother is being weaned off the pain killing opioid drug tramadol. Her mother asks for these tablets very often. She’s hardly been eating since being in the hospital and before that too her daughter says. The hospital doctors have been reducing her dose and she is constantly feeling miserable and depressed. Her GP has been prescribing the drug for her for a long time, which the hospital are not at all happy about. On one afternoon her daughter is visiting and says they are waiting for her son-in-law who works in mental health and will talk to the doctors about what should happen next. “She shouldn’t have taken so many of those pills” her daughter says “but I couldn’t get her off them. I really did try”. The next time when I visit, her mother has been moved to some other unit.
Cathleen is an Irish lady, who’s in the bed right next to Florence. She’s been in a few weeks and is up and about. Cathleen fell over getting into bed one night at home and was on the floor all night, until a neighbour found her in the morning. She is much better now and is waiting for care to be arranged before she can go home. Her family come along to visit several times in the afternoon and she tells her grandson that Florence is 105. “Bloody hell” he says in a very loud voice and keeps coming over to look at my mother and shake his head with what seems to be an admiring and unbelieving smile on his face. Cathleen is able to walk around and likes helping people, she sometimes walks up and down the ward with the lady who is looking for her husband. Cathleen and I talk quite a lot, partly because I’m sitting very near her armchair and also, I think she’s pretty bored.
“I try to help as much as I can” she says and she does. She’s often picking things up for people and helping them take lids off their dinner plates and reach their drinks and tissues. She talks to me in quite a conspiratorial way, she often begins with an apology for what she’s going to say. “I’m going to tell you something and you know I wouldn’t lie don’t you” or “I’m not being funny, I’m not being nasty, you know what I’m saying, I just tell it like it is”. About the lady with one tooth, she tells me on the first day I’m there “she thinks she’s going home but she’s not, she says it every day”.
Cathleen’s husband is in a nearby care home where he’s been for a while. This turns out to be the one my mother will finally go into. So, I get to see Cathleen again weeks later and it’s a real pleasure. It feels like catching up with an old friend.
The next week when I visit, the man down the corridor is still shouting for help. Cathleen has gone home as care twice a day has been found. There’s a new lady in her bed. She looks full of life, except that she is very thin and frail. She is quite stylish in a dark pink nightie and over gown with a colourful scarf tying up her dark hair. I find out later she’s 95 and called Joan. She has a smart phone and a tablet which she uses all the time. Her daughter, she tells me lives in the US and has children in their thirties, she’s lived in the US for many years. Joan’s son died of cancer some years ago and her husband long before that. She seems to have no self-pity – and is very alert. She talks to family and friends on the phone with the microphone on and seems not to mind that all around hear her conversations. I learn that her sister-in-law who she’s calling in Canada has a large lump on her leg, she thinks it’s a ganglia and she cannot bend it. Joan encourages her to talk to her doctor about it. The sister-in-law has also got a problem with old income tax returns and Joan tells me later that she goes regularly to her local library to meet with a volunteer who helps her sort out her financial stuff. Joan is very supportive towards her sister-in-law both when she’s talking to her on the phone and when she talks to me about her afterwards. Indeed I learn over the few days that I see Joan that she is sympathetic and helpful to everybody she talks to on her phone or tablet. She’s realistic too and chivvies them along. Its very impressive to listen to her.
Joan tells me that she’s had a fall and has also been ill on and off for a long time. She has lost a lot of weight and eating is difficult and slow. The doctors think she has some sort of stomach problem and she is in for more tests. She tells me it was really hard for her when first her husband and then her son died and before that her brother and sister-in-law had emigrated to Canada and her daughter to the US. She was sad about it “But you have to make the most of what you’ve got” she says to me. “ I facetime on my computer once a week with my sister-in-law and once a week with my daughter and it’s wonderful. It’s like having them in the room with me. I have to use my tablet or my phone now I’m in hospital” she says “It’s not as good but it’s alright”.
My mother Florence sleeps or dozes through whatever is going on. I am not sure how much she is aware of what is going on around her. She does seem to rouse a little when some of the noise gets to quite high volume, which it does every now and then. But it doesn’t seem to cause her any anxiety or irritate her very much. She opens her eyes sometimes, looks around a little and then closes them again. I speculate that perhaps it’s reassuring that there is life going on all around her.
On one day that I spend with her in the hospital an elderly lady has been admitted into Florence’s side ward that night after having had a fall probably the day before. She’s in quite a lot of pain and in plaster she has to be moved hourly and she screams out quite a lot. I talk to Florence and stroke her hand while this is going on but no real distress seems to register.
On one day when I’m there, a woman’s voice can be heard calling out from a nearby side ward. She shouts “Where am I ?” or “What’s going on?” or “Why am I here?” and sometimes “What am I waiting for?”. I hear the nurses and sometimes the doctors talking to her and trying to explain what’s going on, she stops for a few minutes but soon starts again.
Its loud and close by and Florence wakes up several times looking around her a little perplexed but closes her eyes after each short wake up. I take my mother’s hand on one of the shouting episodes and say to her “mum don’t worry about it, it’s a lady who’s just come on the ward. She’s a bit confused and doesn’t know where she is or what’s happening to her. I expect you probably know what she’s feeling”. A small smile grows on my mother’s face and for a moment she really engages with me “don’t I know it” she says before dozing off again. These little moments of what feels like real engagement happen occasionally between me and Florence or between Florence and whoever is visiting her, be it family or the nurses and doctors who are looking after her. Sometimes in these small exchanges she looks as if she really understands what is being said to her, but she finds it difficult to respond beyond a smile, or a slightly startled look. Even her usual response of “ I’m alright thank you” does not come as easily after a week or so.
When Florence had first arrived at the hospital having broken her leg she was much more ‘with it’. Though for some considerable time before that she had been getting much more frail both physically and mentally. Nevertheless, on her admission to the first ward after fracturing her leg, she had been assessed as possibly being suitable for rehabilitation and perhaps even returning home to her flat in sheltered accommodation. During her stay in hospital she had sadly but perhaps very understandably become increasingly weak.
In the last weeks of her stay on the ward her care team decided that hospital was not an appropriate place for her to be any longer. She was reassessed and it was decided not surprisingly, that she would not be able to benefit from a rehabilitation programme. Rather after some discussion, they considered that she would need to move into a care home offering 24 hour care with regular nursing input.
There then followed a rather tortuous period of searching for a suitable care setting. I was introduced to a care finder who was attached to the NHS and knew an incredible amount about the local facilities available. But there were very few vacancies in places that she thought were suitable for Florence and that were willing to take on a frail 105 year old.
Then out of the blue the care finder rang me one Friday afternoon. A place was available on a ward within what she described as a very good care home but a decision had to be made quickly. When I pushed her a bit more on it she said “It’s the sort of place I’d like my mother to go to if she ever needed it”. She was quite excited and also told me that the manager had been thrilled when told my mother’s age. That was quite a clincher and my sister and sister-in-law went around to see it on the Sunday and luckily quite liked it too. The hospital though very careful not to push the fact that they badly needed her bed, obviously did and Florence was moved in a few days later.
Florence was there for just over two months before she died very peacefully. The care home and the staff were indeed quite wonderful throughout her stay.
As I talked about in my last story, we were later to thank our and her lucky stars that this was all happening before Covid19 had caused such awful trauma for so many care home residents and their families and for the amazing people who look after them.